From time to time, NSF receives inquiries about a condition called flat back syndrome. To find out more about it, Nancy Schommer recently interviewed Michael LaGrone, MD, a scoliosis specialist who has a private practice in Amarillo, Texas. Dr. LaGrone is a member of the Scoliosis Research Society and a medical advisor to the NSF. He is also a member of the clinical faculty of the Texas Tech University Health Science Center.
Q: Dr. LaGrone, what is flat- back syndrome?
A: Flat-back syndrome is the loss of lumbar lordosis of the spine after one has scoliosis surgery. The normal lumbar curvature becomes flat, or you may even get a reverse curvature (called lumbar kyphosis). The condition is characterized by the inability to stand up straight, and typically patients will have back pain in their upper or lower spine. It can occur in patients of any age, but it is more likely to be found in older adults who have had scoliosis surgery.
Q: What causes the condition?
A: The most common cause is the use of distraction instrumentation such as a Harrington rod, in the lumbar spine. Obviously, the patients who have the most severe flat-back syndrome will be those who have had distraction instrumentation placed all the way down to the sacrum. Occasionally, we will see patients who have thoracolumbar kyphosis-a deformity above the lumbar area which would aggravate the forward positioning of the spine and cause flat-back syndrome. But far and away the most common etiological factor would be the use of distraction instrumentation in the lumbar spine.
Q: What are spine surgeons doing about this?
A: Most-but not all-spine surgeons now know that this is something you don’t do. In the early days of scoliosis surgery, surgeons were more concerned with the frontal plane of the deformity and were not as aware of the sagittal or lateral plane, and over time they began to see patients presenting with these problems. It soon became apparent that the sagittal plane was just as important as the frontal, and we realized the importance of not using distraction instrumentation in the lumbar spine. As a result, the incidence of flat-back syndrome has diminished, but we still see it.
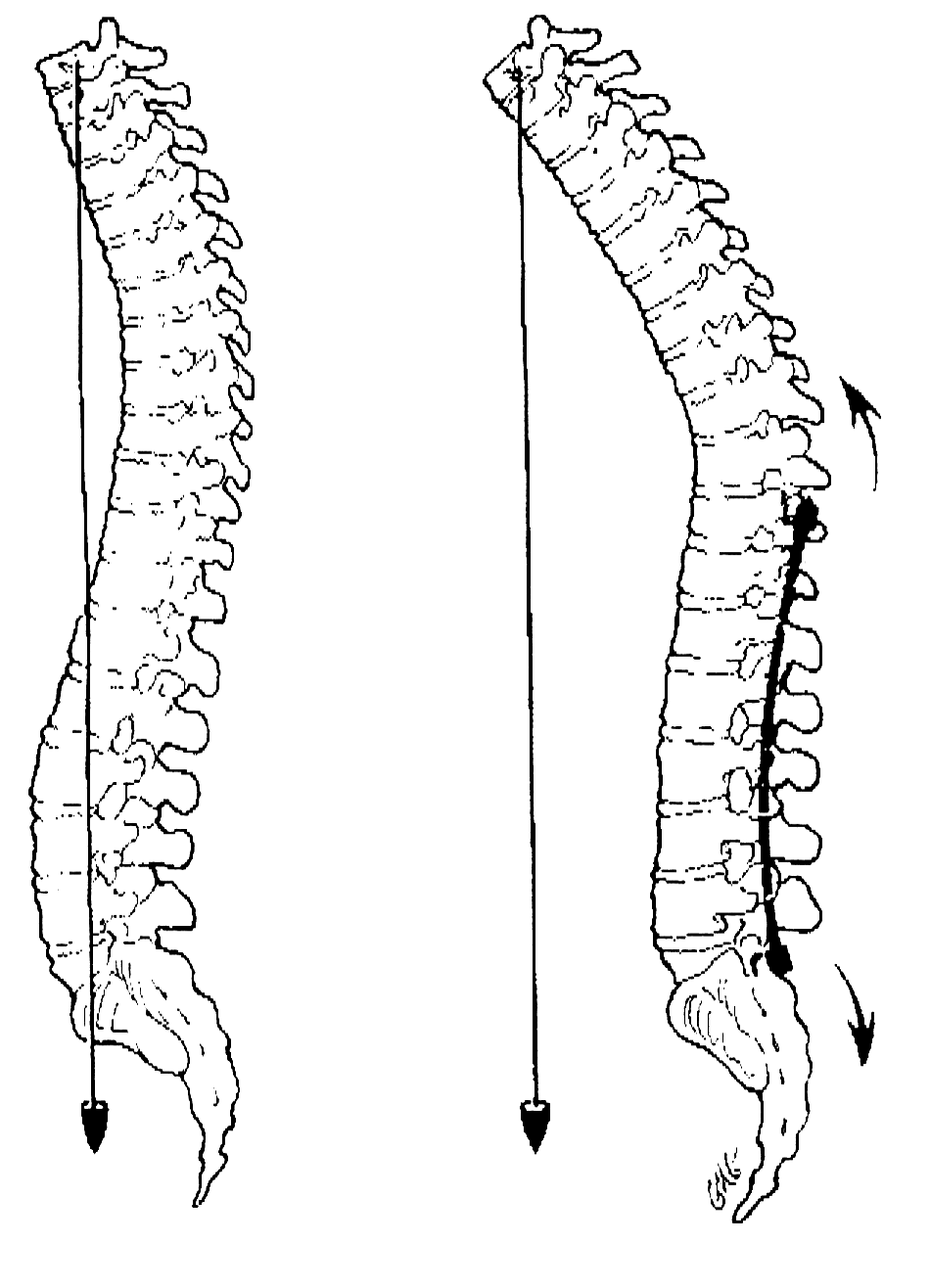
Despite contouring for lordosis, the lumbar spine can be flattened by the force of s distraction rod(arrows). Also note the kyphotic deformity just above the rod. (click image to enlarge)
Q. When would a patient realize he or she had flat-back syndrome? Immediately after surgery?
A: Actually, the syndrome is usually noticed over a gradual period of time and can worsen. The distraction rod will immediately flatten the spine but some patients can compensate for it by extending their upper spine or extending their hips. Over time they can become more symptomatic-they may lean forward more or they may lose hip flexibility. And if their fusion wasn’t solid to begin with, they’ll gradually lose even more of their lordosis.
Q: What can be done about flat back syndrome?
A: Prevention is the key, by which I mean avoiding the use of distraction instrumentation in the lumbar spine. Today we use segmental, instrumentation systems with multiple hooks, wires and pedicle screws. These enable us to maintain the normal sagittal contours of the spine.
Q: In addition to using segmental instrumentation, what else are surgeons doing to prevent this problem?
A: We know the importance of maintaining the patient’s lordosis during surgery. We do that by positioning patients with their hips extended so that we can preserve the lordosis while we are performing the surgery.
Q: What is the surgical treatment for flat-back syndrome?
A: Surgical treatment is very complex and complications are high. Typically, we do what are known as closing wedge osteotomies: we remove wedges of bone from the fusion mass and close the wedges down so that we can re-establish the lordotic curvature. Generally, patients do better and have a higher fusion rate if we precede the osteotomies with an anterior discectomy and fusion of the lumbar spine. Then we do our posterior osteotomies and use rigid segmental instrumentation to maintain correction.
Q: After surgery, what can patients expect?
A: In older adults, I would probably recommend wearing a lightweight protective brace for 6 to 9 months while the spine is healing. For adolescents, a brace might not be needed if the internal fixation is rigid enough.
Q: Do many patients suffer from complications after the surgery to correct flat-back syndrome?
A: In one of our studies, done in 1988, we found that 47% of (55) patients continued to have some symptoms of leaning forward and 36% continued to have moderate to severe back pain. Thankfully, our results are better today because of our increased knowledge and improved techniques.
Q: What should patients do if they have flat-back syndrome?
A: The majority of those who have mild to moderate flat-back syndrome will probably be fine-they’ll be able to keep their spine balanced by compensating for it above their fusion or below, and by keeping fit. It’s difficult to predict whose flat-back will get worse, so it’s a good idea to monitor patients every year or so. If the condition is already severe, and the individual is unable to stand erect, that patient will probably be a candidate for surgical correction.








